 Planning a surgery suite used to be fairly simple. General operating rooms (ORs) were used for a wide range of procedures and dedicated operating rooms were limited to cardiac surgery and orthopedics. At the same time, interventional radiologists and cardiologists created their own workplaces. Today, planning surgical and endovascular suites is complicated by the convergence of diagnostic imaging and surgical procedures, rapidly changing technology, increasing specialization, and strict distinctions between operating rooms and procedure rooms. From a facility planning perspective, the number, size, and specialization of ORs and endovascular procedure rooms is the single most significant factor contributing to the overall footprint of the suite (and project cost). Moreover, the numbers and sizes of related patient care and support spaces are driven by the number and types of operating/procedure rooms. More importantly, the number of operating/procedure rooms drives ongoing staffing and related operational costs.
Planning a surgery suite used to be fairly simple. General operating rooms (ORs) were used for a wide range of procedures and dedicated operating rooms were limited to cardiac surgery and orthopedics. At the same time, interventional radiologists and cardiologists created their own workplaces. Today, planning surgical and endovascular suites is complicated by the convergence of diagnostic imaging and surgical procedures, rapidly changing technology, increasing specialization, and strict distinctions between operating rooms and procedure rooms. From a facility planning perspective, the number, size, and specialization of ORs and endovascular procedure rooms is the single most significant factor contributing to the overall footprint of the suite (and project cost). Moreover, the numbers and sizes of related patient care and support spaces are driven by the number and types of operating/procedure rooms. More importantly, the number of operating/procedure rooms drives ongoing staffing and related operational costs.
Surgery/Special Procedures
Factors Affecting the Size of a Surgery Suite
The hospital surgery suite has undergone revolutionary change over the past several decades. For a long time, the focus has been on shifting surgery to a lower-cost outpatient setting. This has been replaced with a focus on lowering both the costs and risks of surgery with the ongoing migration from invasive to less-invasive surgery or noninvasive procedures. Minimally-invasive, image-guided, robotic, and telesurgery ― along with intraoperative imaging techniques ― continue to replace traditional surgical procedures. Aside from the economies of scale achieved with larger surgical suites, the biggest single factor contributing to the overall footprint of the surgery suite is the size and specialization of the individual operating rooms (ORs). Other factors include the proportion of outpatient surgery performed in the suite, and the type of patient care spaces provided, as well as the efficiency of the surgical suite layout.
Estimating Surgery Space Based on the Number of Operating Rooms
Sometimes a preliminary space estimate is needed to evaluate location alternatives, conduct a feasibility study, or develop a preliminary cost estimate for construction or renovation. Once the number of operating rooms (ORs) is determined, an estimate of the total footprint required for the surgical suite can be made using the rules-of-thumb in this post.
Estimating Space for an Endoscopy Suite
Endoscopy procedures — using a rigid or flexible scope to examine the interior of a hollow organ or cavity in the body — may involve the upper gastrointestinal tract (GI endoscopies), large intestine (colonoscopies and sigmoidoscopies), lower respiratory tract (bronchoscopies) and the urinary tract (cystoscopies) along with a variety of other specialized procedures. Endoscopy procedures generally take 30 to 45 minutes. Patients are usually given intravenous sedation and may recover for up to an hour after the procedure. Recovery time has been reduced significantly in recent years due to the use of shorter-acting sedatives.
Smart Operating Rooms Are Coming to Community Hospitals
Smart technology is ubiquitous today but the best example in the modern hospital is the smart operating room (OR). Once found in only a few large academic medical centers, the technology is showing up in the surgical suites at mid-sized community hospitals like the 344-bed Sacred Heart Hospital in Eau Claire, Wisconsin. Just a few years ago, it was unthinkable that a community hospital like Sacred Heart Hospital could be one of the first in the country to use a technology configuration that includes the iCT (intra-operative computed tomography) and iMRI (intra-operative magnetic resonance imaging) for both diagnostic and surgical use. At Sacred Heart Hospital, patient treatment using advanced technology has improved quality out-comes and reduced the need for additional surgeries. It also has given the hospital state-of-the-art tools that have enabled it to draw top medical and surgical talent to the region.
New Intraoperative Imaging Solutions for Neurosurgery
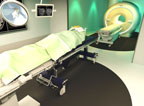 Removing as much of a brain tumor as possible during neurosurgery can make a critical difference in preventing recurrence. Philips has introduced a new MR-OR intraoperative neurosurgery solution based on its Ingenia MR system that allows a neurosurgeon to quickly perform a magnetic resonance imaging (MR or MRI) scan to check the results of a resection during the surgery and remove additional tumor mass if necessary — without first closing the patient’s skull. This reduces the number of repeat surgical procedures, shortens hospital stays, and improves neurosurgery success rates.
Removing as much of a brain tumor as possible during neurosurgery can make a critical difference in preventing recurrence. Philips has introduced a new MR-OR intraoperative neurosurgery solution based on its Ingenia MR system that allows a neurosurgeon to quickly perform a magnetic resonance imaging (MR or MRI) scan to check the results of a resection during the surgery and remove additional tumor mass if necessary — without first closing the patient’s skull. This reduces the number of repeat surgical procedures, shortens hospital stays, and improves neurosurgery success rates.
